Despite a surge of panic about Ebola in the United States, health experts believe the single most effective way to combat the disease is to focus America’s attention on West Africa. But leading aid groups warn that staffing shortfalls, logistical challenges and other bottlenecks could undermine efforts by the U.S and its partners to fight the virus overseas.
The U.S. has devoted more resources than any other nation to fighting Ebola, committing more than $350 million in aid to the region. The U.S. government has also pledged to send up to 4,000 troops to the area to build Ebola treatment centers in Liberia, the country hit hardest by the outbreak.
RELATED: More travel restrictions announced as Ebola ‘czar’ starts
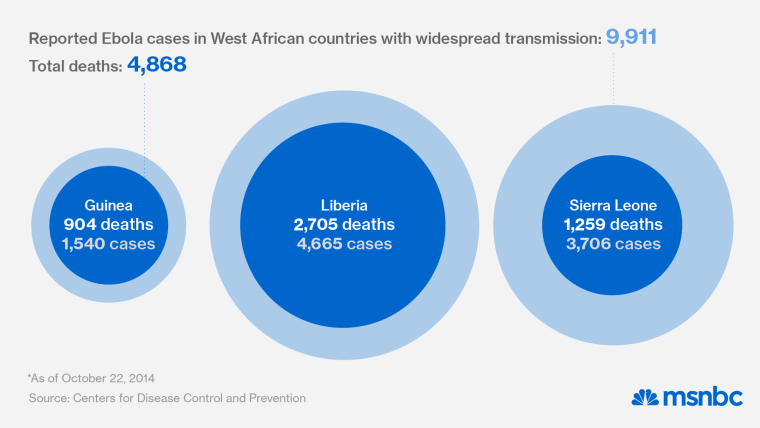
Ebola has crippled West Africa's already fragile health care system, increasing the urgency for outside assistance. Nearly 100 health care workers have died of Ebola in Liberia, according to the World Health Organization. Overall, the WHO says there have been 9,900 Ebola cases and 4,900 deaths to date, though the group acknowledges that the actual number is likely much higher because of under-reporting.
"The fire is burning out of control."'
Concerns about the Ebola response in West Africa go beyond finances. “It’s not just money—it’s how to mobilize what is available as quickly as possible. The fire is burning out of control,” said Jennifer Kates, director of global health policy at the Kaiser Family Foundation.
Sophie Delaunay, executive director of Médecins Sans Frontières (Doctors Without Borders) in the United States, praised the U.S. government for the scale of its response in West Africa. But Delaunay is concerned that staffing shortages could hamper the containment efforts.
RELATED: Ebola continues its deadly march
The U.S., for example, has committed its troops to building 17 Ebola treatment units with 100 beds each in Liberia. But neither the U.S. Department of Defense nor U.S. government health workers will be directly managing or running them.
“The U.S. did not have a willingness to have the [Department of Defense] run these facilities, which for us is a matter of concern. They want to identify the NGO (non-governmental organization) and other partners to take care of these aspects. But we believe it will be impossible for them to find these sufficiently skilled staff,” said Delaunay, whose group has been leading the fight against Ebola in West Africa.
"We really need to convince the U.S. government to take a greater part in the management and running of these centers,” she added.
Given the politics surrounding Ebola in the U.S.—and the concern about endangering U.S. troops—it's an unlikely outcome. Before approving funding for the mission, U.S. lawmakers demanded that the Obama administration provide assurances that the health of American troops would be protected.
"As a few thousand of our troops will be sent into harm's way, I am deeply committed to continuing to conduct rigorous oversight of this mission to ensure our men and women are provided the protection they deserve," Oklahoma Republican Sen. James Inhofe said Oct. 10. The White House originally requested $1 billion for the operation, but Congress chose to approve $750 million instead, as lawmakers like Inhofe said the administration did not have a sufficient plan for transitioning out of the region.
Officials from the U.S. Agency for International Development (USAID) say that the Liberian government, with assistance from the WHO and countries like the U.S., will take the lead in finding staff. “We are confident, working in support of the government of Liberia, that all planned ETUs (Ebola treatment units) will be staffed appropriately with medical professionals, trained health workers and support staff,” said Matthew Herrick, spokesman for USAID, who estimated that “anywhere between 80-90% will be sourced locally.”
“There are lot of people in Liberia willing to work and just need to be trained,” Bill Berger, who leads the U.S. government’s Ebola response team in West Africa, said in a phone interview from Liberia. While the U.S. military won’t be directly staffing the units, it will train local residents to work in them. Berger believes such efforts will help Liberia become more self-reliant in the long term as well, “so they can fight Ebola if there’s an outbreak in the future."
The need for adequate staff is critical: A single 100-bed treatment center needs 200 staff and costs about $1.1 million to run, according to Rebecca Milner of the International Medical Corps, another aid group working in the region. Just putting on, taking off and disposing of the personal protective equipment is labor-intensive, and each suit can only be worn for an hour or two at a time, given the region's climate, she explained.
"There is concern with the fact that because the deployment is slow, the outbreak is actually ahead of us."'
The entire West Africa region will need 19,000 additional doctors, nurses and paramedics by Dec. 1 to fight the epidemic. But convincing others to come help has been a serious challenge, said Delaunay. “It’s not easy to find human resources in this context. It’s scary—there is a lot of stigma around Ebola.” USAID is appealing for qualified health workers to volunteer in West Africa through its website.
There have also been delays in opening a 25-bed hospital for health care workers in Liberia, which the U.S. government is also constructing. Officials hope the hospital will help encourage more aid workers to help on the front lines of the epidemic, particularly as the facility will be staffed by 65 officers from the U.S. government’s public health service commissioned corps. But the hospital's opening has now been pushed back from mid-October to early November. The first ten Ebola treatment units will be rolled out between mid-November and mid-December—also later than originally expected.
The delays have frustrated some working to combat the epidemic on the ground. “I am not criticizing the military, not criticizing the president, but what I’m saying is the hospital isn’t working yet,” said Ken Isaacs of Samaritan’s Purse, a Christian aid organization whose medical director, Dr. Kent Brantley, is an Ebola survivor who contracted the disease while working in Liberia.
Isaacs was in Liberia helping to deliver supplies two weeks ago, when he said there was still a lack of transportation and logistical support on the ground.
The epidemic has continued to defy predictions about the scale of the response necessary in West Africa, which has made rapid mobilization even more urgent, said Delaunay of Doctors Without Borders.
“There is concern with the fact that because the deployment is slow, the outbreak is actually ahead of us,” she said. “The amount of beds, treatments needs are higher than what we had estimated at the time and what has been committed.”

Among other things, Isaacs wishes that American troops would arrive more quickly. Currently, 617 U.S. military personnel are in the country, in addition to 171 civilian staff.
“We are very thankful for the hundreds that are there. If the military came in a muscular and robust, vitalized way—with their capacity, having trained people, they would have a profound impact. But it appears that they’re either unprepared or there’s some kind of delays that are going on,” said Isaacs.
U.S. defense officials say that the rollout has been timed to avoid overwhelming Liberia’s infrastructure. “We’ve been asked why there aren’t greater troop numbers in Liberia at a faster rate, but there’s only so much impact that Liberia and the infrastructure can take from the U.S. military,” Pentagon spokesman Navy Rear Adm. John Kirby said last week. “We just can’t go in there lock, stock and barrel without thinking about the impact on their own infrastructure.”
Berger, the USAID official, believes the Ebola response is gaining momentum and will continue to do so as it scales up. “What we’re seeing is that events on the ground are having an impact already. We’re guardedly optimistic that we’re bending the curve here in Liberia,” he said. The U.S. has increased the number of safe burial teams—a critical step given how quickly dead bodies transmit infection. The U.S. is also creating new mobile testing labs, setting up an airbridge for supplies in Senegal, and supplying personal protective equipment, among other efforts. The military has also brought four Osprey helicopters to help with transport in the region.
Bergen feels particularly encouraged by the emergence of empty beds at the heart of the epidemic. Both international aid groups and U.S. officials in Liberia say there have been more empty beds in treatment centers, in contrast to the overflowing wards earlier in the crisis. But those leading the fight, including Bergen, caution that it’s too early to conclude that this is a definitive sign that the epidemic is beginning to ebb.
RELATED: Pentagon launches Ebola rapid response team
“The trend is very difficult to follow. We’ve seen the numbers down, only to see number spike later,” said Delaunay. While the empty beds could be a positive sign, it may also indicate that sick patients are having trouble reaching the isolation units and are being cared for in their homes, she noted.
There have been more definitive signs of progress in some neighboring countries: Nigeria was declared Ebola-free this week, thanks to the country's more developed health care system and other resources. But International Medical Corps, which is working closely with the U.S. government in West Africa, says it’s critical that the U.S. continue the momentum at the heart of the epidemic.
“Sometimes with world events, there’s an announcement and a flash in the pan. This one is too critical to the global community—you can’t lose your intensity and focus,” said IMC's Milner.
"America and nowhere in the world is going to be safe is this spins out of control in Africa."'
U.S. lawmakers are now mulling additional aid to the region and are lobbying other nations to contribute more, as the global response has fallen short of the need. The United Nations has estimated that $988 million in humanitarian will be necessary to combat the epidemic, which the WHO says could reach up to 10,000 new cases per week by December. Slow to respond in the early months of the epidemic, the international community has committed only 42% of that figure to date, and the U.S. alone is responsible for one-third of that aid. Within the U.S., private donations for Ebola relief have been slow to come in as well.
But U.S. political debate has focused instead on travel bans on visitors from West Africa—a move that experts say would deliver a devastating blow to the flow of supplies and workers, at a time when commercial airlines are already scaling back flights. "All the discussion about travel bans—it's just a very clear signal that we don’t care about you, we only care about ourselves," said Lawrence Gostin, a professor of global health law at Georgetown University.
Delaunay believes that U.S. leaders need to make it clear to the public that the Ebola fight in West Africa should be the country's priority. “I don’t want to minimize the anxiety that is existing in ... the U.S. But it is the responsibility of policymakers to re-balance the state of affairs and put a little bit of reason and reasoning in,” said Delanay.
She added that Doctors Without Borders has been “overwhelmed by requests from U.S. hospitals telling us, ‘What are your protocols, we don’t trust the CDC.’” (Doctors Without Borders signed off this week on tighter Ebola guidelines that the CDC issued for health care workers, but Delaunay said the group’s own protocols borrow significantly from the U.S. agency.)
If the disease remains unchecked, experts worry that it could reach a larger urban center in Africa, then leap to India or China, with catastrophic results. “There are potentially hundreds of thousands of cases over there. The [American] public and political community are not putting this in perspective,” said Gostin, who believes that the international community has relied too heavily on aid groups like Doctors Without Borders.
"They're on the ground, providing all the care, taking all the risks. We’ve asked them to do far too much as a charity—this needs to be a responsibility of the international community," Gostin said. "America and nowhere in the world is going to be safe is this spins out of control in Africa."